Health
My Gut, My Rules: How I Found Peace Without Crazy Diets
Sick of restrictive IBS diets that don’t work? Discover how learning to listen to your gut—not follow extreme plans—can help restore comfort and control with IBS.


I Tried Every Diet for IBS—Until I Stopped
Low FODMAP. Gluten-free. Dairy-free. Keto. No raw foods. No legumes. No fun.
If you’ve been diagnosed with Irritable Bowel Syndrome (IBS), chances are you’ve tried at least one (or five) of these diets. So did I. And each one promised relief—until they didn’t.
What I ended up with wasn’t just a list of “safe” foods. It was fear. Social anxiety. Nutritional deficiencies. And worst of all: a disconnection from my own body.
But that changed when I shifted from control to understanding—from “what not to eat” to “why am I reacting this way?”
The Truth About Diets and IBS
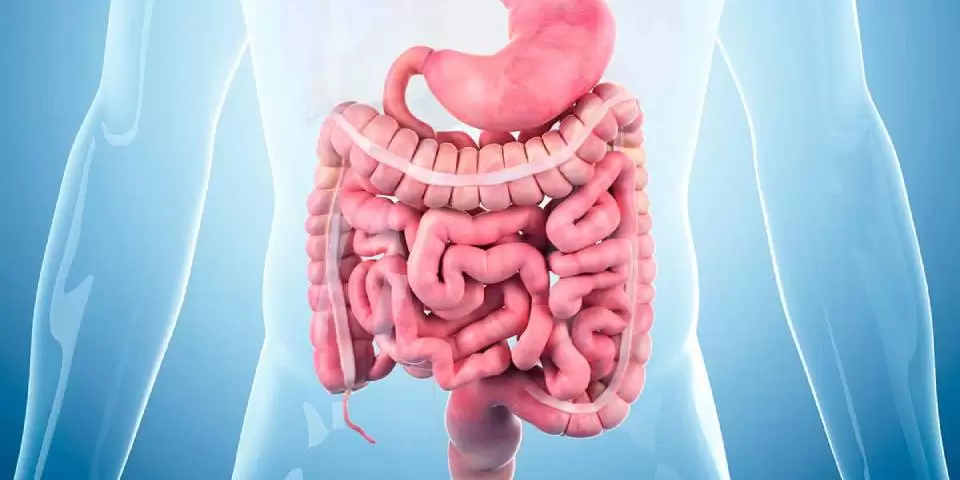
Extreme restriction isn’t always the answer. Here’s why:
- IBS is highly individual. What triggers bloating or diarrhea in one person might be completely fine for another.
- Over-restriction can backfire. Studies have shown that long-term use of elimination diets can disrupt the gut microbiome and lead to nutritional imbalances.
- Stress impacts digestion. The mental load of constantly fearing food can worsen IBS symptoms via the gut-brain axis.
In short: no one-size-fits-all diet will “cure” IBS. But building a relationship with your gut might help you manage it better than any rigid rulebook.
How I Found My Balance—Without Losing My Mind
Here’s what worked for me (and many others who’ve grown weary of endless rules):
1. Identified Core Triggers Gently
Instead of eliminating 30 foods, I started with a food and symptom journal. I noticed patterns—not dogma.
2. Introduced Targeted Probiotics
Using a spore-based probiotic, like Bacillus coagulans, helped improve my digestion from the inside out—making my gut more resilient to small indulgences.
3. Focused on Gut Support, Not Deprivation
I added foods that supported gut lining (like soluble fiber, bone broth, and fermented foods I tolerate), instead of just removing “bad” ones.
4. Let Go of Guilt
Some days, I ate the cookie. Some days, I didn’t. I stopped labeling food as “sinful” or “clean”—and my gut got quieter as my anxiety did too.
The Science Supports a Balanced Approach
According to a 2021 review in Frontiers in Nutrition, personalized and moderate dietary adjustments paired with microbiome support are more effective and sustainable than harsh elimination diets for long-term IBS management.
The study also emphasizes the role of gut microbial diversity and psychological well-being in managing symptoms.
“My Gut, My Rules” Means I’m in Charge
I no longer follow someone else’s checklist.
Now, I ask:
- “How did this food make me feel?”
- “Did I enjoy this meal emotionally and physically?”
- “Is this a rule… or a fear?”
If it helps, I keep it. If it hurts, I reconsider. But the rules come from my experience, not someone’s blog or TikTok challenge.
Final Thought
You don’t need to starve joy to survive IBS.
You don’t need to be perfect to feel better.
And you definitely don’t need to follow 28-day resets, juice cleanses, or ultra-strict plans to reclaim your digestive peace.
If your gut has been yelling at you, maybe it doesn’t need more rules.
Maybe it just needs to be heard.
Looking for a gentle, science-backed way to support your gut—without the diet drama?
GutShields – Liquid Spore Probiotic delivers stable, targeted strains like Bacillus coagulans SNZ 1969® to balance your microbiome naturally.
No restriction. Just smart support.
Because your gut deserves calm—not chaos.
Health
Hydration Hacks for IBS: The Right Way to Drink Water
Drinking water the wrong way can worsen IBS symptoms. Discover how to hydrate smarter—small sips, steady timing, and natural add-ins—to support digestion and gut balance.

“It’s not just about drinking more water—it’s about drinking the right way.”
If you have Irritable Bowel Syndrome (IBS), you’ve probably been told to drink plenty of water. But here’s the catch: how you drink matters just as much as how much you drink.
For many people with IBS, chugging large amounts of water in one go can actually trigger strong intestinal contractions, leading to urgency, bloating, or discomfort.

The Science of Hydration and Digestion
- Rapid intake of water can overstimulate the digestive tract and speed up motility.
- Even, steady hydration supports smoother digestion and nutrient absorption.
- Proper hydration also helps regulate stool consistency, easing both IBS-C (constipation) and IBS-D (diarrhea).
In short: your gut doesn’t just want more water—it wants consistent hydration.
Practical Hydration Habits for IBS
Here are science-backed ways to drink water that keep your digestion steady:
✅ Sip, don’t chug
Aim for 150–200 ml (about half a cup) every 2 hours instead of gulping down large amounts at once.
✅ Infuse with digestion-friendly add-ins
A slice of lemon, cucumber, or fresh mint can make hydration enjoyable and may help soothe bloating.
✅ Match timing with meals
Drink water between meals rather than during them to reduce the risk of overwhelming your stomach acid and slowing digestion.
✅ Choose temperature wisely
Many people with IBS find that room-temperature or warm water is gentler on the gut than ice-cold water.
The Bigger Picture

Hydration is one piece of the IBS puzzle. Pairing good hydration habits with microbiome support—such as spore-based probiotics like GutShields—creates a powerful daily foundation for calmer digestion.
Bottom Line
When it comes to IBS, hydration isn’t just about volume—it’s about rhythm. Steady, mindful sipping can keep your gut balanced and your symptoms calmer.
✨ Stay hydrated, stay balanced—let GutShields help protect your gut microbiome.
Health
Why Sleep Quality Can Make or Break Your IBS Recovery
Poor sleep doesn’t just cause fatigue—it can worsen IBS by raising cortisol, triggering inflammation, and disrupting gut bacteria. Learn how to improve sleep to support your digestion and long-term gut health.

“Poor sleep isn’t just making you tired—it might be keeping your gut inflamed.”
Living with Irritable Bowel Syndrome (IBS) means constantly balancing stress, diet, and lifestyle to avoid flare-ups. But one factor often overlooked is sleep quality. Many people with IBS report that their symptoms are worse after nights of poor sleep. Science now shows this isn’t just coincidence—sleep has a direct influence on the gut-brain axis, the microbiome, and inflammation levels.
If you’ve tried dietary changes, supplements, and even medication without lasting relief, improving your sleep could be the missing piece of your IBS recovery.

The Science: How Sleep and IBS Are Connected
- Cortisol and inflammation
- Poor or fragmented sleep raises cortisol, your body’s main stress hormone.
- Elevated cortisol has been linked to increased gut permeability (“leaky gut”), more inflammation, and heightened pain sensitivity—all of which make IBS symptoms worse.
- Gut microbiome disruption
- Studies show that even short-term sleep deprivation reduces microbial diversity.
- A disrupted microbiome may lead to more gas, bloating, constipation, or diarrhea in IBS patients.
- Gut-brain axis imbalance
- Your digestive tract has its own nervous system (the enteric nervous system).
- Poor sleep dysregulates this system, which can throw off motility—causing irregular bowel habits, urgency, or spasms.
In short, sleep doesn’t just recharge your brain—it recharges your gut.
Practical Steps for IBS-Friendly Sleep

Here’s how you can start improving sleep quality—and by extension, your digestion:
✅ Set a consistent bedtime and wake time
Your circadian rhythm influences gut motility. Going to bed and waking up at the same time each day helps regulate bowel function.
✅ Limit screens at night
Blue light from phones and laptops suppresses melatonin, making it harder to fall asleep. Try switching to a book or listening to calming music.
✅ Create a wind-down ritual
Deep breathing, light stretching, or journaling can signal your nervous system to shift into “rest and digest” mode—essential for people with IBS.
✅ Support with natural aids
Chamomile tea, magnesium glycinate, or lavender aromatherapy have been shown to improve relaxation and sleep quality.
✅ Feed your microbiome wisely
Avoid late-night heavy meals, alcohol, or excess caffeine. Pair your routine with spore-based probiotics like GutShields to support a resilient microbiome overnight.

The Bigger Picture: Sleep as IBS Medicine
When you consistently improve your sleep, you’re not just preventing fatigue—you’re:
- Calming inflammation
- Helping good bacteria thrive
- Regulating gut-brain communication
- Supporting more regular, pain-free bowel movements
That’s why sleep isn’t just a lifestyle tip—it’s a therapeutic tool for IBS recovery.
Bottom Line
If you’ve been treating IBS only through diet or medication but ignoring your sleep, you may be missing a key part of the solution. By protecting your nights, you protect your gut.
✨ Give your gut the rest it deserves—combine better sleep with GutShields for faster, lasting relief.
Health
The IBS-Friendly Morning Routine That Can Calm Your Gut All Day
Your morning choices can set the tone for your gut health all day. Discover a simple, IBS-friendly routine that supports the gut-brain axis, reduces inflammation, and promotes comfortable digestion.

What if the way you start your morning could determine whether you spend the rest of your day in comfort—or in pain?

For people with Irritable Bowel Syndrome (IBS), mornings can feel like a gamble. One wrong choice—whether it’s a cup of strong coffee on an empty stomach or skipping breakfast entirely—can trigger bloating, cramps, or urgent bathroom trips that last all day.
Emerging research shows that morning routines influence the gut-brain axis, the two-way communication system between your digestive tract and nervous system. This axis controls motility (how food moves through your intestines) and regulates inflammation—both of which are key players in IBS.
A calm, balanced start can keep your gut in “rest and digest” mode rather than fight-or-flight, reducing the likelihood of flare-ups.
Your IBS-Friendly Morning Blueprint

1️⃣ Drink Warm Water Before Anything Else
Hydration supports smooth bowel movements and helps “wake up” the digestive tract without the jolt of caffeine. Warm water can be especially soothing for intestinal muscles.
2️⃣ Practice 5 Minutes of Deep Breathing
Deep, diaphragmatic breathing activates the parasympathetic nervous system, which encourages healthy digestion and reduces gut hypersensitivity. Try inhaling for 4 counts, holding for 4, and exhaling for 6.
3️⃣ Have a Gentle, Protein-Rich Breakfast with Soluble Fiber
Instead of skipping breakfast or eating ultra-processed carbs, choose:
- Soft scrambled eggs with a side of cooked oats
- Smoothie with lactose-free yogurt, chia seeds, and banana
Soluble fiber from oats or chia seeds helps regulate bowel movements, while light protein stabilizes blood sugar and supports muscle repair.
4️⃣ Avoid Caffeine First Thing
Coffee immediately after waking can overstimulate the gut and worsen diarrhea in IBS-D, or cause cramping in IBS-M. If you enjoy coffee, try having it after your breakfast to lessen the impact.
Why This Works for IBS
- Hydration + soluble fiber = easier, more regular bowel movements
- Deep breathing = calmer gut-brain signaling
- Balanced breakfast = steady energy without blood sugar spikes
- Delayed caffeine = reduced gut motility shocks and inflammation risk
Over time, these habits can train your body to start the day in digestive balance—meaning fewer flare-ups and more freedom to enjoy your day.

Start tomorrow with these small changes—and discover how calm your gut can be. Pair it with GutShields to support your microbiome from the inside out.
-
 Health8 năm ago
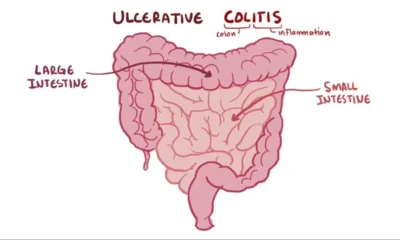
Health8 năm agoAll About Microscopic Colitis: Causes, Diagnosis, and Treatment
-

 Entertainment8 năm ago
Entertainment8 năm agoI Tried Medication, Diets, and Meditation — And Finally Found Peace in Acceptance
-

 Health8 năm ago
Health8 năm agoWhat Is a Gastroenterologist? When to See One, and the Problems They Can’t Help With
-
 Health8 năm ago
Health8 năm agoTop 7 Questions to Ask Your Gastroenterologist!
-

 Health8 năm ago
Health8 năm agoWhat Causes Mucus in Your Stool—and Why You Shouldn’t Ignore It
-
 Health8 năm ago
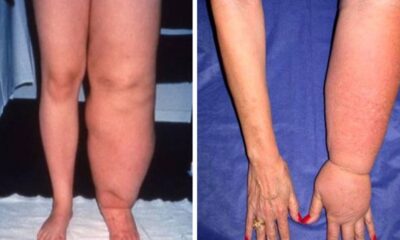
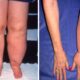
Health8 năm agoA New Cause and Treatment for Lymphedema
-
 Health8 năm ago
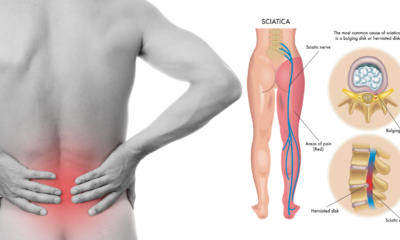
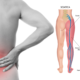
Health8 năm agoIBS and Sciatica Pain – Is There a Connection?
-
 Tech8 năm ago
Tech8 năm agoHealing IBS Isn’t About Forcing Your Gut—It’s About Resetting Its Natural Rhythm
















